~ by Dr. Neville Wilson
Ankyloglossia, or tongue-tie, is a congenital oral cavity anomaly, affecting between 4% to 10 % of infants, and is characterized by an abnormally short, thick or tight, sublingual frenulum, often causing restricted latching to the maternal breast, with adverse feeding outcomes for both infant and feeding Mum.
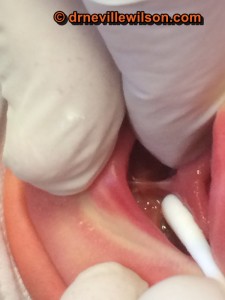
Breast feeding difficulties may arise as a result of poor, or ineffectual, latching, giving rise to an unsettled or dissatisfied infant, who may dribble, reflux, or exhibit signs of early fatigue, frustration, disinterest, or poor weight gain.
Not infrequently these difficulties may be compounded by heightened maternal anxiety, which may be transferred to her struggling infant, aggravating further attempts to breast feed successfully.
Other features of a poor latch may be a clicking of the tongue, or chewing of the nipple, resulting in painful breasts, often leading to nipple cracks, poor breast emptying, and not infrequently to mastitis, thereby impeding further attempts to breast feed.
THE FRENULUM:
The fraenum, or frenulum, is a narrow fold of mucous membrane that connects a moveable part of the body to a fixed part, and the lingual frenulum helps to stabilize the base of the tongue without restricting tongue movement.
It forms the attachment between the underside of the tongue and the floor of the mouth, and is a remnant of the initial attachment of the tongue to the floor of the mouth before birth. (1)
Normal tongue movements include tip elevation, retraction, grooving and protrusion, and provide for suckling, chewing, eating, drinking, clearing the mouth and speech function. Tongue-tie may inhibit these natural movements.
BREAST FEEDING PROBLEMS:
Tongue-tie is unlikely to be detected in bottle fed babies, since the complex movements of the tongue required for latching, extraction and swallowing, are not required when artificial feeding from a bottle is presented to the infant mouth.
It is likely that tongue-tie has not been widely recognized over the past 3 or 4 decades because of the low incidence of breastfeeding in Ireland, largely due to national cultural habits, and the over- enthusiastic promotion of formulae feeding in Hospitals by nursing staff.
While breastfeeding rates in Ireland continues to be lower than in neighboring European countries, there appears to be a discernable reversal of this historical trend, linked to the increasing emergence of lactation supporting groups, and the promotion of breastfeeding by lactation consultants.
Lactation Consultants (LC) are registered nurses who have gained additional training and experience in infant feeding difficulties, and are more likely to recognize and correctly diagnose tongue-tie than other clinicians.
Referrals to our Tongue-Tie Clinic are invariably made by LC nurses on behalf of breastfeeding mothers.
With more Irish Mums opting to breastfeed an increased incidence of tongue –tie diagnosis is inevitable, placing a greater burden of responsibility on nursing and medical staff, and supportive structures.
Reports from the Growing Up in Ireland Study revealed breastfeeding rates in Ireland to be as low as 56% compared to 90% in other European countries.
While some Mums express frustration with lack of support for breast- feeding while in hospital, others will report satisfaction with encouragement by nursing staff.
An investigative report by the Economic Social and Research Institute (ESRI) concluded that Irish mothers need greater support than currently being provided if they are to succeed with breastfeeding efforts after discharge from maternity wards.
Prof Richard Layte (ESRI) is critical of the under funding for breast-feeding promotion by the Government, while Prof Atul Singhal, at University College London, calls for a greater promotion of breastfeeding programs, citing breastfeeding as a major public health issue.
Current research supports the view that breast-fed babies are likely to have lower risks for obesity, diabetes and cardiovascular problems, compared with their formula-fed counterparts, and are less likely to be overfed by having a slower rate of weight gain.
Controversies about the safety and efficacy of tongue-tie division in new born babies with feeding problems prompted the National Institute for Health & Clinical Excellence (NICE) to review justification for tongue-tie division, and to provide guidance in this regard to clinicians in the UK in 2005.
NICE concluded that there were “no major safety concerns about division of ankyloglossia” and that “limited evidence suggests that this procedure can improve breastfeeding”.
BENEFITS OF TONGUE-TIE DIVISION:
My personal experience supports the view that division of ankyloglossia can significantly improve breastfeeding, when latching is impeded, with immediate benefits for infant and Mum.
Dolby and Associates, in a study of 25 mothers of healthy infants with ankyloglossia, reported a significant decrease in nipple pain after frenotomy. (2)
In a random selection of 100 mothers who attended our Tongue-Tie Clinic, all reported a significant decrease in nipple pain, as well as improved latching and successful breastfeeding, following infant frenotomy.
Not every case of tongue-tie requires intervention, and some babies appear to manage to latch effectively despite the restriction.
These babies are likely to thrive since changes in the oral cavity during the first 4-5 years of life will permit the tongue to grow and narrow, causing the lingual frenulum to receded and stretch to the degree that lingual movements are no longer impeded.
CLASSIFICATION:
Tongue-tie may be classified according to its anatomical presentation and severity of stricture, and defined by various classification systems.
In simple practical terms a Type1, or anterior restriction, binds the tip of the tongue to the floor of the mouth, while Type 4 defines a posteriorly restricted frenulum. (Kotlow Diagnostic Criteria).
Type 1 restrictions are easier to diagnose and divide, while clinical experience requires the detection and release of a posterior tongue-tie.
A posterior Tongue-Tie may not be readily identified by a superficial examination of the mouth, and these are often missed by failure to examine the base of the tongue correctly.
Careful palpation of the inferior base of the tongue may reveal the restricting frenulum and facilitate its division with improved lingual function.
There may be slight bleeding following the surgical intervention, but this invariably ceases when the infant is put to the breast.
Tongue-Tie may in some cases be aggravated by a lip-tie, in which a tight upper labial frenulum inhibits the natural flanging of the upper lip and restricts effective latching.
In these cases an altered nursing position may facilitate improved latching. Failure to achieve this may require surgical division of the lip tie.
Frenotomy is a low risk procedure and may on occasions give rise to a small bleed which invariably resolves when the infant is put to the breast.
Mothers are comforted prior to the procedure, and counselled regarding the low risks and potential benefits, and informed that no pain is experienced by the infant.
Some infants will sleep throughout the procedure.
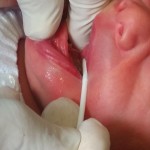
(Below are photos of baby Max who was unable to latch effectively until his frenulum was released, providing instant relief for his Mum who had severely cracked and painful nipples and a good latch for Max with a successful feed.)
SPEECH IMPAIRMENT:
It is speculated that untreated tongue-tie may cause speech impediments in later life.
While medical opinion is divided on this there are adults who report articular difficulties because of failure to divide their restricted tongues in infancy.
Tongue-tie may restrict the articulation of vowels such as T,D,Z,Th,and L. (3)
The emergence of Tongue-Tie Clinics in Ireland is testimony to the growing recognition that the restricted frenulum is more common than suspected, and that relief for these babies and their nursing Mums is now available.
Dr. Neville Wilson.
Medical Director, The Leinster Clinic.
Maynooth.
www.leinsterclinic.ie
11 Sept., 2015.
REFERENCES:
1. Arch Otolaryngeal Head & Neck Surgery 2000, 126:36-9, Messner, A H.
2. J Paed Surgery 2006; 41: 1598-6000.
3. Arch Otol 1971; 94:948-57.


Sorry in advance for the long comment..! I had my second baby a few months ago in Clonmel. My first baby was premature and breastfeeding didn’t work out for us, so when I went over with this one I didn’t think I’d have a problem!
One of the nurses checked her out when she was born and told us she wasn’t tongue tied. That night, after hours of trying to feed her and feeling like a failure, I gave her a bottle and she slept for about two hours. I kept trying to breastfeed after that but she just wasn’t getting anything from me. I felt like I wasn’t doing it right because any time I asked for help a nurse would come and say “the latch is fine, it should be alright now”, and leave. I went home after 2 days and on the last day baby was so tired she slept for over 6 hours without looking for a feed. I felt like the nurses were judging me for giving her bottles and not trying hard enough but nobody actually tried to help. I just put it down to hormones though, I know they’re busy. A pediatrician checked her out before we left and said all was fine.
I gave up breastfeeding at 4 days after a lot of tears (hers and mine!) but she was still having trouble with bottles. It would take 2 hours to feed her every 3 hours. When she was 4 weeks old, my mam tried to feed her and could tell straight away that she was tongue tied! It never even entered my mind before that because I was told she didnt have it. So I started googling and found Dr. Wilson recommended on a blog about tongue tie. I also found out that there’s a doctor in Clonmel hospital that specialises in the division procedure and that we could have had it sorted before we went home, had anyone noticed! Cue more crying for a few days.. stupid hormones! There was no way I was going back there so I rang Dr Wilson’s clinic and got an appointment almost immediately.
I brought her to the clinic and he found that my baby had a type 2 tongue tie and sorted her out there and then. He was very sympathetic and angry for me that I had to go through that for so long and put me at ease throughout the procedure.
She now drinks her bottles in under half an hour and sleeps up to 6 hours a night!
Thank you Angela.
I hope that your testimony is helpful to hospital staff and to the many Mums who are struggling to breast feed their infants. Careful examination of baby’s mouth and tongue is crucial before discharge from hospital, and I am being told repeatedly by Mums that this is not being done.
We need to make doctors and Paediatricians more aware that tongue tie is a very real problem, and not just a “fad” as reported by some family doctors !
Myself and my wife brought our daughter to Dr.Willson as she had a tongue tie that was detected by peadetrican in St.Lukes hospital Kilkenny.what I would like to know is why are these poor baby’s not having there tongue ties done in there local hospitals.we had. To travel to Maynooth from thomastown co.kilkenny to have this procedure down on a 12 day old baby,the Irish health system is that of a third world country an absolute disgrace.we highly recommend Dr.Neville as the procedure was done on seconds and he explained everything before hand to put our monad at rest
I am so happy to have had the opportunity to relieve Georgia of her tongue -tie at the early age of 18 days, Kristian ! And thank you for your comment !
Georgia had a Type 2 Tongue Tie, which was an obvious impediment to breast feeding, causing her to go onto Formulae feeding. You reported that the Paediatrician told you and April “not to worry about it” which was an unfortunate assessment, so I am pleased that you did worry about it and took measures to have the problem rectified. I trust that she is thriving and happy Kristian !
I had my second baby in mullingar hospital while there I found baby Alex was struggling to latch correctly to his bottle , dribbling a lot, and not drinking very much. On the day I was discharged the baby doctor checked him over I expressed concern about Alex feeding he throughly checked Alex mouth, tongue , roof of his mouth and I was told all was fine. When I got home had a visit from public health nurse I discussed with her about feeding again she examined Alex and informed me that he was tongue tied and that i should make an app with dr Wilson asap. I got app with dr Wilson straight away. He explained procedure to us in full he then examined Alex and told us that he had a type 2tongue tie and would benefit from having procedure done. Since having it done Alex is feeding like a PRO. We would like to thank dr Wilson and all his team at the Leinster clinic!!
It was a pleasure to help Alex, Sarah ! And what joy to see him having such a good feed after all his previous struggles. I hope your experience and testrimony helps to convince the skeptics that tongue tie is a very real impediment to successful feeding, and can so easily be remedied with relief for Mum and baby ! He is a lovely little man ! I hope he enjoys his icecream when he is old enough to give it a good lick !
I can not thank Dr Wilson enough for his amazing work with my son seàn. Sean is my 3rd child and I had noticed he found it very difficult to take his bottle as a result of tongue tie.I was told his tongue tie wasn’t bad but I decided I wouldn’t take any chances when it came to my child.as a primary school teacher I have come across so many children who have speech impediments as a direct result of tongue tie. One such case was a 7year old who spent the first two years of his primary school education attending speech and language therapy. Sean has had his tongue tie procedure done and is doing great.I noticed a difference straight away and I would advise any mother or father who is any way undecided as to what to do with their babies tongue tie to seek the professional advise of Dr Wilson. He is an excellent doctor who gives you time before and after the procedure. I would recommend getting this Non invasive procedure done to prevent problems in later life with speech.
Thanks again Dr Wilson
A true gentleman.
I am delighted to have had the pleasure of assisting Sean with his feeding problem Catriona, and wish you both well as you engage in the joy and magic of bonding together !
I had my first baby a week ago and after a difficult birth, I found myself struggling to breast feed my son. After delivery, it took 4 midwives over an hour to get my baby boy latched on for his first feed. Having no experience with breast feeding, I was unaware that the intense discomfort I was feeling was not normal. Later that night, after I had been transferred to the ward, I was spending nearly an hour each time trying to latch on my baby. A midwife assisted me through the night, with varying levels of success. Each feed was becoming more painful than the last, but not once was my son checked for tongue tie, instead the diagnosis for the problems latching was how hard his delivery was. As the days passed, feeding became excruciatingly painful. I was bleeding, covered in cracks and blisters. I had even tried one or two bottle feeds, but baby was struggling to fully latch on to the bottle. Feeling utterly defeated, exhausted and intense pain, I contacted a lactation consultant, Mairead Murphy, who was able to note a possible tongue tie and recommend I see Dr Wilson. Finally today we got the confirmed diagnosis AND solution. My baby boy had a Type 4 tongue tie, which is both difficult to diagnose and not always as easy to see. A very swift procedure performed by Dr Wilson and as if by magic, my baby can latch on not only instantly, but completely pain free. I feel a HUGE sense of relief and a new found confidence that I can finally start to enjoy feeding times and that I will have the freedom to go out and about knowing I can easily breastfeed when my baby is hungry. Dr Wilson’s knowledge, experience and understanding is second to none. Thank you so much for providing me with the miracle I was so desperately looking for! I would highly recommend any other mother feeling the same frustrations to contact Dr Wilson for a check for tongue tie.
I found out my little girl was tongue-tied when the visiting mid-wife was asking how my feeding was going. It was difficult. My baby was slow to gain weight and taking over an hour to feed. After struggling for a few weeks and being referred into Temple Street because she hadn’t reached her birth weight by three weeks, I decided to book an appointment with Dr. Wilson. She was 5 weeks when myself and my husband brought her to the clinic. Dr.Wilson explained how tongue-tie can affect breastfeeding, both mothers and babies. He explained the procedure and checked to see the degree of severity. The whole appointment took no more than 20 minutes and afterwards she fed quicker and better than before. Over the following weeks her feeding continued to improve. We still had to attend Temple street for a few weeks. The doctor said they were not good at picking up tongue-tie and when she could see the improvement passed comment that there must be something to the tongue- tie as an impairment.
We are very happy with the outcome and would recommend Dr.Wilson to check for any tongue -tie concerns.
Hi Dr Wilson, I just wanted to say thank you again for your help with our baby’s tongue tie. After you did the procedure for us, breastfeeding was immediately better and since then we are experiencing the joy of breastfeeding that we so longed for. I have written a post all about our breastfeeding journey and tongue tie procedure over on my blog, http://www.sweetlc.blogspot.ie, I hope you will have a look. Kind regards, Holly
Thank you Holly ! I do congratulate you on your determination to breast feed Andrew, even under the trying condition of his tight frenulum, and I am delighted that you have overcome this unfortunate impediment to natural breast feeding that is so frequently misdiagnosed and untreated.
You have given Andrew the best start to his life and he will benefit immensely from your perseverance and decision, and enjoy the best health benefits that breast feeding offers.
Your Blog is interesting, and hopefully will have formative value for other Mums with a similar problem. Well done Holly !
I had my first baby in 2011 in the Coombe Hospital. From the first latch I had pain & discomfort whilst breastfeeding. As a first time mother I persevered and within a few days I had severely sore, cracked & bleeding nipples. I sought advice from numerous midwives in the hospital who told me that pain was to be expected and to keep going as it would improve as my nipples toughened. It didn’t. Everytime my baby cried my body would shake uncontrollably and I cried through all feeds. Eventually after 3 weeks of exclusive breast feeding, we stopped. I felt an enormous amount of guilt on stopping, I felt like a failure and believed I was a tough, capable person who should have been able to feed her baby. After all, mothers are ‘designed’ to feed and it should be a natural instinct! At my six week visit to a G.P., my son was diagnosed with a posterior tongue tie. I was informed it wasn’t serious enough to be remedied and as I wasn’t feeding him myself now there was no point in carrying out the procedure. I was so angry that it took six weeks to be diagnosed after being seen by many health care professionals in that time period.
I had my second child 2 years later in the Rotunda Hospital . I again endeavoured to breastfeed my daughter and again had constant pain. No tongue tie was ever diagnosed but now, looking back, I am almost certain she had one. After a severe case of mastitis in both breasts I had to stop. I was emotionally and physically exhausted and was struggling to manage a very boisterous 2 year old!
I had my third child on the 1st of July this year. I am more determined the ever to feed him myself for a longer period than the previous two. From the 1st latch, I felt pain. Armed with information and knowledge, I approached the midwife on duty and told her that I had a concern that he was tongue tied. She checked his mouth and told me he didn’t. I persevered with the feeding throughout my hospital stay and was in pain during every feed. I asked the paediatrician to check for a tongue tie as I still had a sneaking suspicion that he had one. The Doctor checked and told me he didn’t. I persevered through painful feeds and told myself it would get better. It wasn’t until a chance meeting with a public health nurse, as my son was crying hysterically, that all my suspicions were confirmed. She asked me if I was feeding him and how was my latch? I told her it was ok and there were a few cracks and ridges but I was ‘managing’! She casually said, ‘you do know he has a tongue tie?’ I felt an immediate sense of relief…I hadn’t imagined the pain. My instincts had been right and yet again it had taken 3 weeks to diagnose, after misdiagnoses from those who should be aware.
She gave me Dr. Wilson’s name as someone who carried out frenectomies. Ironically, Dr. Wilson had been my trusted G.P. a few years back when I lived in Meath. I made an appointment with him and he confirmed Sam had a posterior tongue tie and carried out the minimally invasive procedure there and then. I fed him straight after in a private room and felt instant relief. I received the utmost professional, informative and kind care from Dr. Wilson.
There has been some pain on one side in particular since the procedure but this is due to the nipple trauma prior to the procedure. The pain is greatly alleviated and I’m more determined than ever to persevere thanks to Dr. Wilson.
I apologise for the long post, but it angers me to think that something so simple can solve a very painful issue. There seems to be a trend of misdiagnosis or dismissal with regards to tongue ties and I’m sure that many women could have continued to breastfeed as intended.
Thank you Dr. Wilson. Debbie, Brian and Baby Sam.
Debbie, it was my pleasure to help you and Brian give Sam the best start to his life.
I am only sad that you had so much difficulty in the past and that your current problem was missed by so many health providers.
I guess this demonstrates how difficult it is sometimes to diagnose a posterior tongue tie, even by skilled professionals.
I am seeing this type of tongue tie with increasing frequency and wonder how many are actually being missed. They are not easily detected and also not always successfully treated, since posterior tongue ties have a tendency to re-attach, often requiring a second or even third frenotomy to achieve lasting success.
Keep up the exercises and best wished for You and Sam as you offer him the best start to life !
To anyone reading this blog with a doubt about tongue tie, get it seen to asap..and for those that have had it released yay to happier feeding and happier babies 🙂
My story…
I’ve a 7 week old and a nearly 4yr old.
Toddler born Dec 12′ was handed to me in delivery ward and after a few mins at starring at him realising he was real and I’d just given birth, I noticed his tongue was funny looking, (I knew nothing about tongue tie) to me all I saw was the stringy bit under the tongue was so close to the edge of his tongue. I asked midwife who said it was normal for small babies. Their tongue grows and it will be fine. As with most new parents Google becomes ur new best friend. I never tried to breastfeed, and as he was gaining weight anytime I queried his tongue it was dismissed. I was told it was tied but “it will stretch” or “at worst he will have a speech impediment” which is where he is now… his tongue is still tied, and his speech is no where near where it should be… If he had of gotten the tie released when he was a baby all this would of been prevented.
Its a waste of mine and my toddlers time… I’ve to do pronounciatin homework with him, which frustrates him. Its a waste of time and money for the hse… This could be used on a child that really needs it… its so infuriating! ! We have now been told as he is over 6 months it’s major surgery to get ut released and they are reluctant to put a toddler through major surgery unless it’s really needed… so now been told that unless a dentist deems it necessary , as he can’t clean his teeth wuth his tongue,food getc stuck in his teeth causing decay then ut will be done… so my poor child needs to have brutal speech and decaying teeth before its done… What a joke!!!
Needless to say when I got pregnant again, I was more clued in and had read that it was most likely heredity so I was armed wuth knowledge and I was going to be strong and not pushed over.
My little boy was born 7 weeks ago and similar to my toddler I noticed the tongue. It was no where near as bad as what toddlers looked but still looked different.
Again on bottles he dribled milk out the side of his mouth at every feed. You could hear him gulping in the wind.asked midwife and paed dr in rotunda, all dismissed the notion of tongue tie. Phn said he had a slight tongue tie but ut should cause any issue. Tbis was when he was 4 days old. I was already having issues with severe trapped wind and a cranky out of sorts baby.
Asked at 2 week check, gp said that the frenulum was tight but it should be an issue and he was just a colicky baby.
Persevered on … changed bottles as I thought that was the issue… changed formula. ..used infacol, changed formula again started using colief droPs. .. All having little to no effect… baby was still screaming in pain 🙁
6 week check and a different gp, and straight away he said he’s TT are we gonna organise to get it released … I nearly started crying. .. I knew he was yet no one was believing me till now. Gp said he would send off a referal to the hosp to get it treated. When he left the nurse advised me to ring Dr. Wilson. .. Was seen by him 24 hrs later,
Baby ollie had severe stage 2 tongue tie. .. released there and then. Quick and seemed painless.
Ollie has been a lot calmer, taking bottles better and is not getting in air like he used to. Brilliant results! !
Going to bring my toddler in to see him , and see what real advice he has regarding his tongue tie, as no body elsee seems to pay attention to it…
The industry as a whole I believe are living in the clouds… they are shoving TT issues under the carpet which causes bugger issues down the road.
It looks like such an easy and straight forward procedure I can’t understand why it’s not done by more ?
Apologies for ranting and raving but it’s a shocking health system we have!!
Thanks Dr Wilson, see you soon with my eldest!
Thank you for your helpful comments Laura ! I do hope that they will be of help to some struggling Mums, and also help to clarify some of the misconceptions that many doctors have about the problems associated with tongue tie in infants who are desperate for an unrestricted and natural feed !
I do trust that Ollie has settled and that he is well and thriving !
I just want to say a big thank you to Dr Willson after diagnosing and carring out the tongue tie procedure to my daughter when she was just five weeks old , it was the best thing we did for her and for me as I was trying so hard to breastfeed her . We had a very tough time before , she wasn’t able to feed herself properly she was losing weight -I was in terrible pain developing cracked nipples and mastites ! Such a shame that her tongue tie wasn’t diagnosed in the hospital when she was born would been such an easy and enjoyable first five weeks rather than going through to all that pain . I really hope that in the near future the hospitals will carry out this procedure when the baby’s are born as no baby should struggle to feed because of the tongue tie! Thank you again , Dr .Willson .
We just want to say a big thank you to Dr Wilson for carrying out the tongue tie procedure on our baby boy, Senan.
We recently had our 4th baby and I was discharged from hospital the day after his birth. The following day I noticed he wasn’t feeding enough or latching on correctly. Feeding was also uncomfortable and painful, something I had experienced with my other children. The day after that I brought him back into the maternity hospital and was advised to top him up with an oz or 2 of formula at every feed in order for him to gain weight. I was then advised that if he became ill to bring him to a children’s hospital. My husband and I were very upset by this. The next day our Public Health Nurse was checking Senan and she diagnosed the tongue tie, thankfully!! She told us about Dr Wilson so we phoned for an appointment straight away and got one for 48 hours later. Dr Wilson was brilliant and very informative. He advised us that our little boy had a type 3 posterior tongue tie, which is pretty bad. I cannot believe the hospital did not check for this. He carried out the simple, painless procedure on our 6 day old baby. Straight away he latched on perfectly and now at 8 weeks old is absolutely thriving.
I advised my GP that every doctor needs to check for tongue tie because if diagnosed early it can be corrected so easily. They took Dr Wilson’s details from me so if anyone else is in the same position as us they can advise them where to go as I would highly recommend him. I’m also very disappointed with the maternity hospital. They took blood tests and monitored our little boy for a few hours and was basically saying he was failing to thrive and the first thing they suggested was formula. Not once did they look in his mouth!! We cannot thank you enough Dr Wilson.
Dérerca, Vinnie & baby Senan.
Dear Dererca and Vinnie,
I am so happy to have been able to help Senan with his feeding difficulty and glad to hear that he is thriving and happy !
Well done on being persistent and best wishes for the future with your lovely little boy !
I had my first baby, Daniel, on 18 October 2017. I was determined to breastfeed and made sure the midwives in the Rotunda hospital were aware of my intentions, ensuring that we had the opportunity for skin-to-skin immediately and to latch the baby to the breast within an hour of his being born. This was all facilitated, but by the morning of his second day, I began to experience severe nipple pain when feeding him. I asked in three separate occasions to see the hospital lactation consultant and was told by the midwives that she was ‘very busy’. I was also told that baby Daniel’s latch looked great (which it did, from the outside) and that my nipples would ‘toughen up’ after a few days. By day 3 the pain was excruciating and I could see cracks on the nipples. Daniel’s nappy contained what looked like a dusty red substance, which I later discovered was a sign of dehydration. I still did not receive a visit from the lactation consultant. The paediatrician examined Daniel on the morning of day 3 and I saw him sweep a gloved finger around his little mouth. He asked how the breastfeeding was going and I told him it was painful. He assured me that this would improve. I asked to go home that day. That evening, I tried to feed Daniel in spite of the pain. Next thing I knew Daniel pulled off the breast and there was blood everywhere (or at least it seemed that way!). I was crying, he was crying, and I immediately resolved to contact Mairéad Murphy, who is a private lactation consultant. She arrived at our house within the hour and gave me a nipple shield to help with the pain. She diagnosed a tongue tie and recommended that we have it seen to by Dr Neville Wilson. As it was a Friday and after hours, we had to wait until Monday to make contact. We were due to have Daniel weighed and seen for his heel prick test the following day. We were told that he had lost 11% of his weight. Luckily, the nurse we saw was a lactation consultant and she did a weighed feed. Daniel was not getting enough milk from the breast so we were advised to hand express and syringe feed him 30mls every 2 hours. This was a huge amount! Not only was it very difficult to get that amount from the breast, but little Daniel’s tiny tummy wouldn’t take all of it! We did our best to get as much as possible into him, as we were told he needed to gain at least 20g in weight by the next day. He was dehydrated and if we didn’t manage it, he would have been taken back into the hospital. Thankfully, he gained 60g! This was helped by Mairéad lending us a pump.
We made an appointment with Dr Wilson to assess Daniel’s tongue tie the following Tuesday. He diagnosed a bad type 3 tongue tie and performed the procedure to release it. He showed us to a quiet room where Daniel latched beautifully and he fed from my breast successfully for the first time. He was 6 days old at this point. My nipples were still injured but the reduction in the pain I was experiencing was immediate. Dr Wilson recommended I use silver breast cups, which sped up the healing process and within about 2 weeks I was able to dispense with the nipple shield.
I cannot believe that Daniel’s tongue tie was not diagnosed when we were in the hospital. I am still angry at being told that the lactation consultant was ‘too busy’ and that even the paediatrician missed Daniel’s tongue tie. So much pain, stress, and suffering would have been avoided were the staff properly trained and made aware of the various symptoms of tongue tie, not just trained to look at the latch from the outside. If there is pain then there is something wrong! Listen to the mother! We were lucky to have had the means to hire a private lactation consultant. If we hadn’t, our breastfeeding journey would never have begun.
We are so grateful to Mairead Murphy and to Dr Wilson for their expertise. Daniel is now just over 3 months old and exclusively breastfed. We intend to continue for as long as possible.
Dear Estelle.
I am delighted to hear that Daniel has done well post surgical frenulectomy.
It is rather disappointing to hear of the poor support you have had at hospital, but I do hope that this trend will soon end as practitioners become more aware of the problem and how easily it can be rectified by surgical release.
I have written to several hospitals outlining the need for a full assessment of oral cavity and tongue movements following birth, and anticipate that in time this may become a routine aspect of the neonatal examination.
Well done on your persistence, Estelle, and good to hear that Danny is thriving !